A gastroscopy is performed to examine the upper digestive tract; this includes the oesophagus, stomach and start of the small intestine. The gastroscopy will investigate symptoms such as swallowing difficulties, upper abdominal pain, heartburn, loss of weight and anaemia.
The patient is sedated (made sleepy) by a qualified anaesthetist who injects a sedative via a cannula (tiny hollow plastic tube) inserted into a vein This is not a general anaesthetic but the patient is asleep.
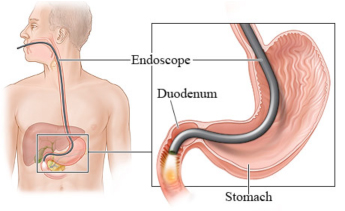
When the patient is asleep a flexible tube about 70cm long and about 9mm in diameter is passed through the mouth and down the oesophagus, passing through the stomach and ultimately reaching the duodenum (start of the small intestine) Throughout the procedure images of the lining of the upper digestive tract are seen in real time on a television screen.
Lesions such as ulcers, polyps, cancers, inflamed areas and abnormal veins, among other things, can be seen. lf necessary, lesions can be sampled by taking a biopsy (a small "pinch" of tissue) to be sent to the lab and examined under a microscope. Some lesions can be completely removed with a snare (a wire loop). lt is also possible to undertake procedures to stop bleeding lesions such as ulcers and abnormal blood vessels.
A standard diagnostic gastroscopy (examining to find a cause for symptoms) takes about 10 minutes and is very safe. After the procedure the anaesthetic drug wears off very quickly and you are given something to eat and drink. Dr Desmond will review you before you go home and discuss with you the examination findings and the follow up plan.
Please don't bring any valuables with you. Wear loose/comfortable clothing as you will be required to change.
Bring your private insurance and Medicare details with you.
Please arrive at the hospital/day procedure centre at your required time.
Feel free to bring something to read or do as your arrival time is not the procedure time. You need to check in and change into a hospital gown, which can take some time. ln addition the time taken for the cases ahead of you can vary depending on complexity so the exact procedure time is unpredictable. Whilst our best intentions are for you to not wait too long, each procedure is unique and sometimes a person on the list in front of you will have an unexpected finding which may prolong their procedure time and your wait.
You can expect to be at your hospital/day procedure centre for approximately 3-4 hours from arrival time to departure. Sometimes this is much faster and we can call your "pick up" person when you are ready to go.
Once in the examination room, the anaesthetist will administer a sedative agent to make you sleepy and comfortable. lt is not a general anaesthetic, but almost all patients are unconscious and have no recollection of the procedure. Occasionally some patients momentarily rouse and may have some recollection of the event. lt is not generally painful.
The time taken to complete the procedure varies, but is generally around 5-10 minutes.
Depending on the findings, biopsies (samples) may need to be taken, or polyps (small growths of the upper gastrointestinal tract lining) may be removed.
After the procedure you will be taken to the Recovery Area until any sedation wears off - it's not uncommon to have some bloating after the procedure or a sore throat. These will both pass over a short time. When you are awake, Dr Desmond will visit you and explain the results of the examination to you. Follow-up arrangements will be made if necessary.
You will be given discharge instructions.
After you have had something to eat and drink you will be able to go home. You are not allowed to drive home, ride a bike or operate dangerous machinery for the rest of the day/night. Do not sign any legal documents or drink alcohol during that same period of time. On the morning of the following day you may resume all normal activities.
Suite 2A/330 High St,
Ashburton 3147
Ph: 9885 8100
Fax: 9885 6495
View on map
Cabrini Brighton, Suite 6
243 New St.,
Brighton 3186
Ph: 9885 8100
Fax 9885 6495
View on map
Cabrini Malvern
Cabrini Brighton
Glen lris Private
Monash Medical Centre